Vitamin D: The Evidence in adults
Click on the appropriate heading below to view full information
Early French trial - Chapuy
Study details:1
Aim: to examine the effects of supplementation with vitamin D3 and calcium on the frequency of hip fractures and other nonvertebral fractures.
Patient study group: 3,270 healthy ambulatory women.
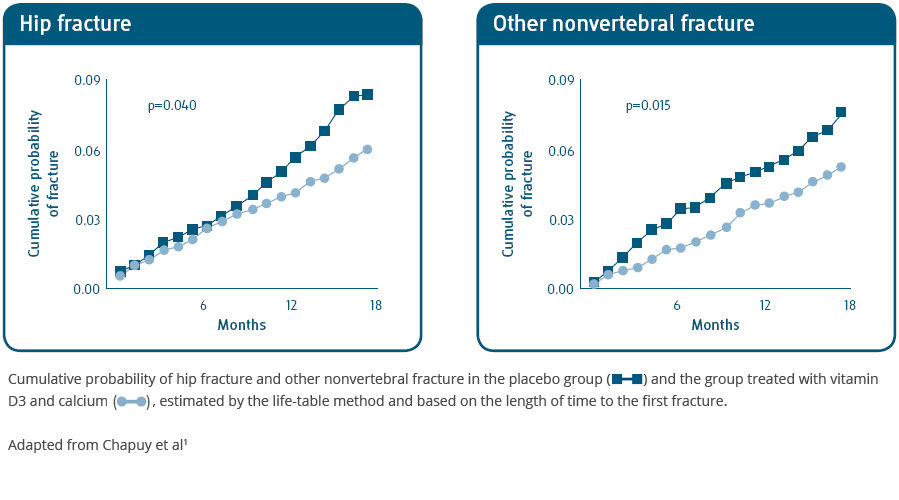
In the vitamin D3/calcium treated group vs. placebo:1
- The number of hip fractures was 43% lower (p=0.043)
- The total number of nonvertebral fractures was 32% lower (p=0.015)
Pivotal US trial: Dawson - Hughes
Study details:2
Aim: to study the effects of three years of dietary supplementation with calcium and vitamin D on bone mineral density (BMD), biochemical measures of bone metabolism and the incidence of nonvertebral fractures.
Patient study group: 176 men and 213 women ≥65 years, living at home.
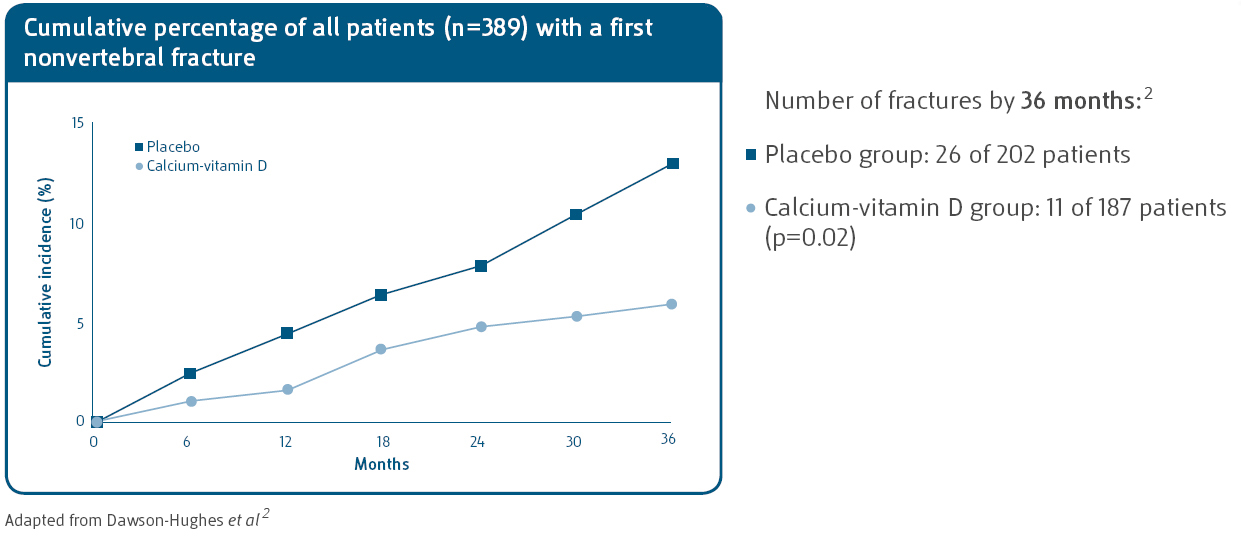
Over the three-year study period from baseline:2
- Moderately reduced bone loss measured in the femoral neck, spine and total body
- Reduced incidence of nonvertebral fractures
1 year intervention study - Hitz
Study details:3
Aim: to evaluate the effect of 1 year of treatment with calcium and vitamin D on bone mineral density (BMD) and bone markers in patients with a recent low-energy fracture. (Unlike other studies, these patients already had a low-energy fracture of the hip, forearm, shoulder or spine.)
Patient study group: 122 patients (84% female)
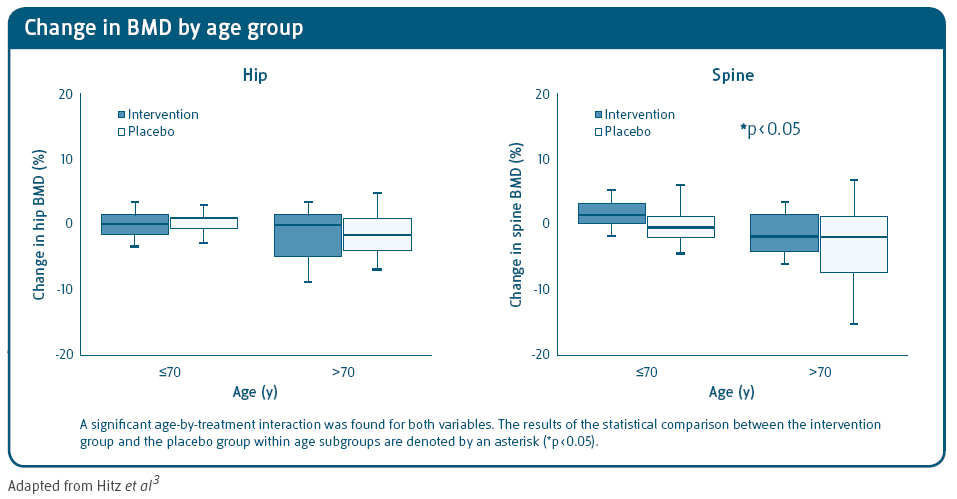
Following 1 year of treatment with calcium and vitamin D:3
- Reduced bone turnover and significantly increased BMD in patients ≤70 years of age
- Decreased bone loss in patients aged 70+
- Patients with hip fracture showed the greatest increase in serum 25(OH)D from treatment: 25(OH)D increased from an insufficient concentration of 33nmol/L to 85nmol/L
Meta analysis: Bischoff - Ferrari
Bischoff-Ferrari’s 2009 meta-analysis demonstrated reductions in nonvertebral fractures with a high dose of vitamin D (482-770 IU/day) compared to lower doses of vitamin D (<400 IU/day)4:
- 29% reduction in nonvertebral fractures in community-dwelling individuals
- 15% reduction in nonvertebral fractures in institutionalised older individuals
The effect was dose dependent and independent of additional calcium supplementation.4
